FRONTIERS IN MEDICAL CASE REPORTS - Volume 4; Issue 3, (May-Jun, 2023)
Pages: 01-05
Print Article
Download XML Download PDF
Erythema Elevatum Diutinum: A Case Report of Presentation and Management
Author: Mark-Young Seadey, Margaret Lartey
Category: Medical Case Reports
Abstract:
Erythema elevatum diutinum (EED) is a rare, chronic necrotizing vasculitis and treatable skin condition, it has many histological mimics and is often association with a variety of underlying diseases. When these are present the management and prognosis dictate the course of EED. This case report highlights the rare nature of the disease, the difficulties encountered in clinching the diagnosis and the treatment and outcomes.
Keywords: Erythema Elevatum Diutinum, Rare Disease, Skin Disease
DOI URL: https://dx.doi.org/10.47746/FMCR.2023.4303
Full Text:
Introduction, Epidemiology and Aetiology
Erythema elevatum diutinum (EED) is a rare chronic skin disease often manifesting as red-brown nodules, papules, or plaques commonly on the extensor surfaces (Yiannias et al., 1992). EED was first described in men in 1888 by Hutchinson (Hutchinson, 1888) and in women in1889 (Bury, 1889). Radcliff-Crocker and Williams in 1894 concluded that the two types should be described as one entity and so gave the name EED (Hutchinson, 1888). Lesions are often asymptomatic, however pain or a burning sensation may be present. The disease is rare and also challenging to diagnose.
The aetiology of EED remains unclear and speculative. Whilst spontaneous evolution is often seen after 5-10years (Hutchinson, 1888), various cases have been reported to last up to 25 and 39 years in association with IgA gammopathy and post cholera vaccination respectively (Bury, 1889; Crocker, 1984).
Systematically most patients are well although arthralgia and constitutional symptoms and may be present (Crocker, 1984). EED can occur at any age with no racial predilection, but most commonly affects patients in their fourth and sixth decade, and it appears to present earlier in those with human immunodeficiency virus (HIV) (Wilkinson et al., 1992). The cutaneous manifestations of EED have many clinical and histological mimics. An accurate diagnosis is important as this can prompt the search for associated conditions that may require monitoring of treatment (Wilkinson et al., 1992).
In order to make a diagnosis of EDD, a skin biopsy is required in to rule out other differential diagnosis. Direct immunofluorescence may reveal changes consistent with vasculitis, deposits of fibrin intravascularly and perivascular, compliment and immunoglobulins (IgG, IgA,IgM). Gammopathies can be identified by immunoelectrophoresis (Yiannias et al., 1992).
In addition to a detailed systemic enquiry, serological testing including full blood count, electrolytes, HIV antigen, autoimmune profile may reveal underlying disorder associated with EED.
Case Report
We present a 59 yrs old man, who presented with a three-year history of nodular growths on the dorsum of the metacarpophalangeal joints, palmar aspects of the hands, the extensor surfaces of the elbows, on the right knee, both thighs and the ears. The above started on the elbows, and gradually increased in size and number to the other body parts mentioned. Lesions were painless and erupted discharging blood and serous fluid. He is a known Hypertensive and adherent to medications and well controlled.
An initial histopathology report of lesions from a biopsy on the right elbow showed a granulomatous dermatitis. An infective cause was favoured and Giemsa stain highlighted small organisms which were considered to be Leishmania bodies, but clinical correlation was lacking.
A second histopathology of biopsy from a lesion on the elbow and from other sites showed features suggestive of an infective process most likely Histoplasmosis. However histopathological diagnosis did not correlate with clinical features of the lesions so a third biopsy was requested which confirmed the diagnosis of EED.
Other investigations done included ANA and Rheumatoid factor which were both negative.
Fungal microscopy and fungal cultures were all negative and PSA level was 0.53ng/ml which was also normal.

Figure 1: Papulonodular eruptions on the palmar surfaces of both hands.
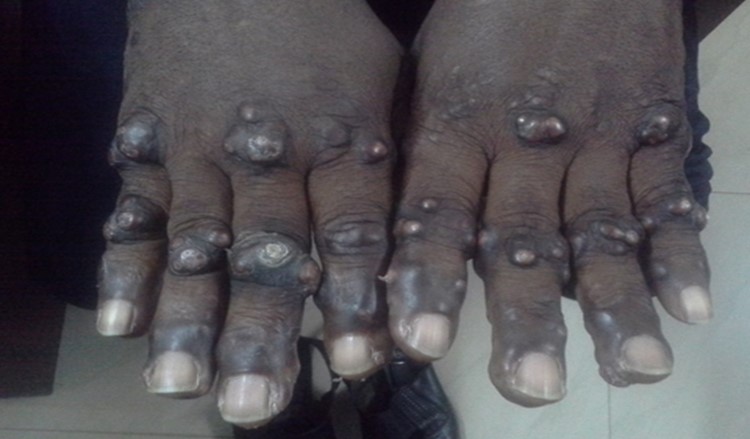
Figure 2: Papulonodular eruptions on the dorsum of the metcarpophalangeal joints.

Figure 3: Flesh colored popular eruptions on the upper arm and nodular eruption on the right elbow.
Treatment and Outcomes
Patient was started on Dapsone 100mg daily which resulted in flattening of the lesions and stopping of spontaneous eruptions. He has been on treatment for a total of eight years. Stock outs of Dapsone, result in regrowth of lesions, the latest occurring in 2020 during COVID-19 lockdowns and. He has routine full blood counts bimonthly to monitor the side effects of Dapsone.
Discussion
EED is a rare form of chronic vasculitis that is usually associated with underlying underlying disease processes such as hematological malignancies, connective tissue diseases, chronic infections, inflammatory bowel disease, HIV and streptococcal infection (Bury, 1889; Crocker, 1984). The present case is unusual in the fact that the patient had no detectable underlying illness. The diagnosis of EED is often delayed and the same occurred in the case described, taking over two years to clinch the diagnosis. The case is also unique in the fact that patient has been taking dapsone intermittently for over 8years since diagnosis with good effect. The differential diagnosis of EDD includes Sweet’s syndrome, pyoderma gangrenosum, granuloma annulare, Kaposi sarcoma and bacillary angiomatosis.
Associations of disease like HIV, hematological disorders, autoimmune disease as these are likely to play a critical role in early diagnosis and management.
Patients with EED usually present with plaques or nodular lesions located at the extensor surfaces of joints. In general patients present between the ages 40 and 60 years of age (Wilkinson et al., 1992). These lesions are often symmetrically located and start as plaques that further develop into nodular lesions.
The histological features of early-stage show polymorphonuclear leukocytes or mixed polymorphonuclear leukocytes with lymphocytes with fibrin deposition in and around the vessel walls, but with little red cells extravasation or other features of vasculitis (Wilkinson et al., 1992).
Therefore, taking into account its chronicity, the potential for misdiagnosis and possible under lying systemic disease: the importance of correct diagnosis is paramount to allow for adequate treatment of underlying systemic disease if needed. Although treatment options are limited dapsone is the mainstay of treatment. Dapsone monotherapy can be regarded as effective in 80% of cases (Momen et al., 2014).
Conclusion
This case report highlights a rare and chronic disease, the difficulty in making a diagnosis and a treatment option with a relatively good outcome with patient satisfaction. Another difference between this case and other reported cases is the absence of a co-morbid systemic disorder. This can help mask the diagnosis. It is hoped that this case will add to data on EED.
Acknowledgements: We acknowledge the patient who not only gave informed consent but encouraged the publication to educate others.
Conflict of Interest: The authors have no conflict of interest to declare
Funding Source: None
References:
Bury JS. A case of erythema with remarkable nodular thickening and induration of the skin associated with intermittent albuminuria. Illus Med News 1889; 3: 145-149.
Crocker HW. Erythema elevatum diutinum. Br J Dermatol 1984; 6: 1-9.
Hutchinson J. On two remarkable cases of symmetrical purple congestion of the skin in patches, with induration. Br J Dermatol 1888; 1: 10-15.
Momen SE, Jorizzo J, Al-Niaimi F. Erythema Elevatum Diutinum: a review of presentation and treatment. J Eur Acad Dermatol Venereol 2014; 28: 1594-1602.
Wilkinson SM, English JS, Smith NP, Wilson-Jones E, Winkelmann RK. Erythema Elevatum Diutinum: A clinicopathological study. Clin Exp Dermatol 1992; 17(2):87-93.
Yiannias JA, EL-Azhary RA, GibsonLE. Erthema Elevatum Diutinum: A clinical and histopathologic study of 13 patients. J Am Acad Dermatol 1992; 26: 38-44
|



